Current State of Healthcare Payment Integrity Systems
Improving payment integrity has been a challenge for health plans since the beginning of time as the constant battle for accurately pricing claims rages on. To help the market better understand the current state of payment integrity and expose the need for alternative approaches to solving payment integrity challenges, HealthEdge® Source recently commissioned independent research firm, In90group Research, to survey more than 100 health plan leaders.
Respondents represented all types and sizes of health plans along with leaders from virtually every department, and here is what they had to say about the current state of payment integrity:
- Multiple third-party editors: 90% of respondents depend on two or more payment integrity vendors. That means they must maintain multiple datasets, update schedules, and sometimes even multiple instances across their lines of business. The IT burden and workflow complexities associated with approach have become overwhelming for many health plans.
- Claims rework: 55% of payers report that greater than 20% of their claims require rework due to inaccurate first-pass adjudication. Not only does claims rework require additional time and effort from the payment integrity team, but it also creates downstream work for other teams, such as provider relations.
- Number of dedicated FTEs: 70% of payers have more than 10 full-time employees (FTEs) dedicated to prospective payment integrity and 45% have greater than 25 FTEs. When asked what the future looks like when it comes to dedicated resources, 56% of respondents said they expect the number of internal FTEs dedicated to payment integrity to growth in the next one to two years. Unfortunately, this comes at a time when workforce shortages are at an all-time high.
Clearly, the traditional approach to payment integrity is not producing the results that health plans want. That’s likely because payers have historically relied on payment recovery vendors to help facilitate prospective payment integrity.
The result? Stacks of editing solutions, ever-expanding contingency fees, and mountains of siloed data sets that provide limited visibility into opportunities for operational improvement. As staff members attempt to hunt for answers across different systems, the time versus value equation begins to erode. Plus, business leaders are unable to identify and resolve root-cause issues across the organization or make more informed business decisions based on comprehensive data.
Payers are rightfully frustrated with the limited progress they are able to make when it comes to payment integrity improvements. Survey respondents shared their top five barriers to success when it comes to payment integrity:
- 64% – Limited resources makes it hard to keep up with fee schedules and policy updates. As both IT and business resources remained strained across the organization, modernizing payment integrity processes and systems often fall behind other priorities, such as changing regulatory requirements that carry hard-and-fast deadlines. But with constantly changing fee schedules and policies – at both federal and state levels, complexities compound and payment integrity improvement initiatives fall further behind.
- 58% – Hiring and retaining qualified resources to perform complex payment integrity tasks. Furthermore, survey respondents expect this problem to persist, as 58% say they must increase the number of manual resources in payment integrity just to keep pace with the demand over the next two years.
- 56% – Limited visibility into third-party vendors’ findings for root-cause analysis. This is likely due to the contingency-based incentive models that payment integrity vendors have in place.
- 43% – Legacy technology is not flexible enough to meet their unique needs. Historically, the focus of payment integrity has been on content, not the technology that enables the content to be accessible across the organization.
- 41% – Conflicting departmental initiatives/ Key Performance Indicators (KPIs) limit ability to improve payment integrity. With payment recovery goals conflicting with payment integrity KPIs, health plans find themselves challenged to make meaningful progress.
Payers are also frustrated with their third-party vendors. When asked, payers shared the following top challenges with their vendors, and the top five most commonly mentioned challenges included:
- 58% – Cost
- 47% – Lack of innovation/upgrades and solutions
- 37% – Limited savings/value
- 32% – Ineffective at getting results
- 27% – Limited content
What’s most concerning about these challenges is that most of these exactly align with the purpose of these types of solutions.
As the complexities of and frustrations with payment recovery and integrity continue to grow, interest in taking a fresh, enterprise-wide approach to improving the accuracy of payments is growing. This is evident in the research findings where survey respondents were asked to choose their top three payment integrity goals through 2025.
Top Goals for Payment Integrity Through 2025:
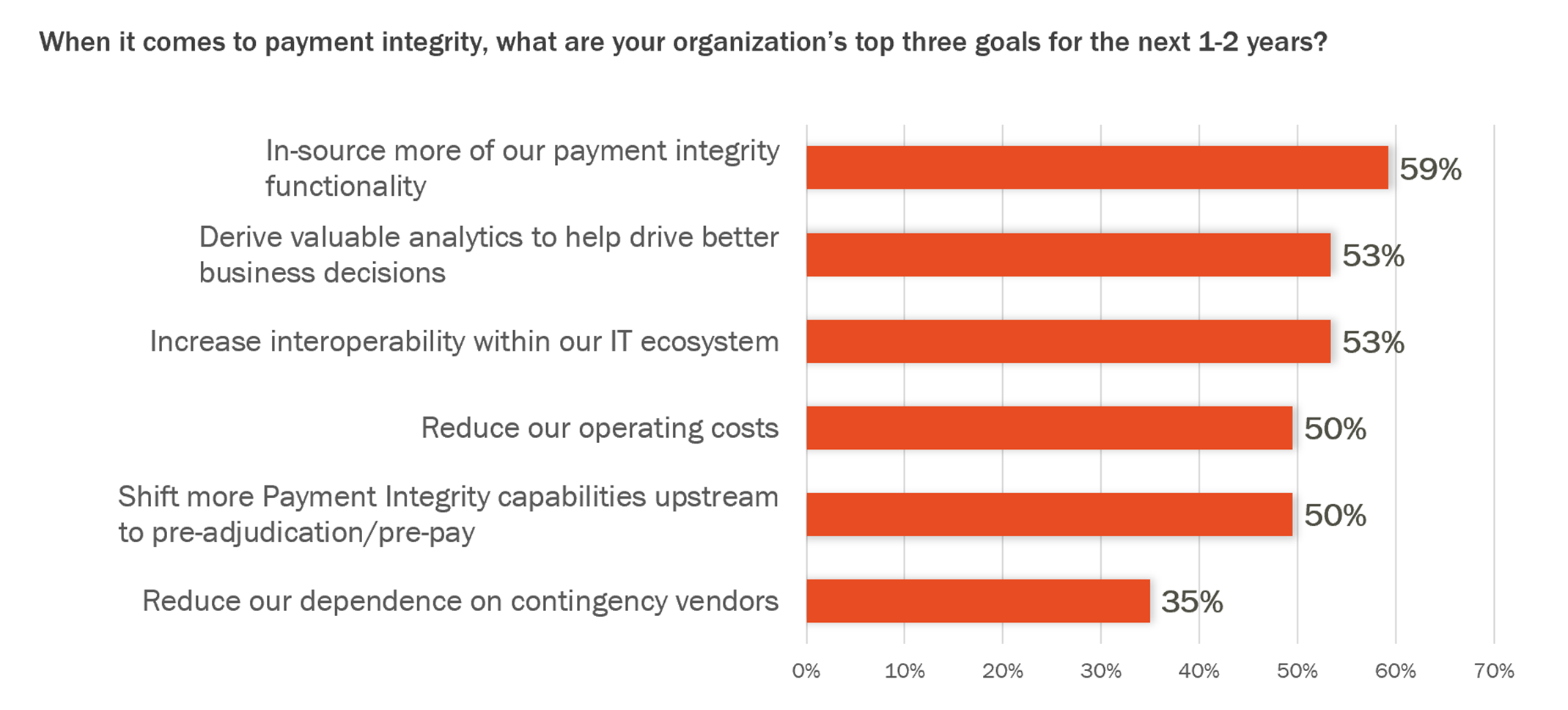
When comparing these top goals to the top challenges health plans face, it becomes clear that health plans must take a thoughtful approach to payment integrity, one that relies on highly interoperable technology solutions that can reduce dependencies on editors, minimize the burden on IT teams, and bring insights together from multiple systems and departments to provide a clearer picture of payment issues across the enterprise.
To learn more about how HealthEdge Source can help your organization rethink your payment integrity improvement strategies to make a meaningful difference in 2023, visit the Source page on the HealthEdge website.
